
News
Introducing Digital Technology is a Priority for Healthcare in the Far East
How does the Ministry of Health plan to further drive the development of high-tech healthcare in the Far East?
At the end of 2018, high-tech healthcare services had been provided to over 34 thousand patients, 21 thousand of which were using mandatory health insurance funds. The basic mandatory health insur- ance programme covers high-tech health services at 84 care providers including 5 federal, 72 regional, and 7 private health organizations.
In 2019, the availability of high-tech healthcare (both covered and not covered by the basic mandatory health insurance programme) in the Far Eastern Federal District was 418.87 treated patients per 100,000 people, compared to a figure of 474.05 in the nation at large. There is obviously room for improvement in the district.
At a meeting with private healthcare executives, we discussed the current state of and prospects for developing nuclear medicine techniques for cancer diagnosis and attracting private funds for building PET centres in Russian regions. According to the executives, PET centres are slated to be opened in three regions of the Far Eastern Federal District: in the Republic of Sakha (Ya- kutia) and in Primorye and Khabarovsk Territories.
The Ministry of Health is consider- ing establishing a reference centre for the Far Eastern Federal District at the Vladivostok Oncology Dispensary. It is supposed to perform image interpre- tation and tissue analysis to provide a more comprehensive diagnosis based on histological, chemical, and immunological parameters.

Are there any additional plans to attract private or foreign partnerships?
Interdepartmental cooperation with Far Eastern countries — China, Japan, and Korea — is developing rapidly.
In September 2016, for example, the Russian Ministry of Health and the Kore- an Ministry of Health and Welfare signed a Memorandum of Intent to Cooperate in Health Information Technologies in Vladivostok. Last year, in June, the Nine Bridges plan for Russian-Korean trade and economic cooperation was adopted in Moscow, providing for the exchange of experiences and training for health professionals at organizations in both countries. Besides that, we are also plan- ning on cooperating in the development of eHealth.
What can we expect from eHealth?
Introducing digital technologies is a top priority for healthcare development. It is actually a crucial pre-condition for the effective functioning of all our sys- tems. In 2017–2018, about a thousand healthcare locations in the Far East were connected to the Internet in the process of building the health data exchange infrastructure. It was paid for through federal funds. We are planning to double that number of connected locations within the next five years.
In 2018, every region in the Far East- ern Federal District integrated into the Unified State Health Information System (EGISZ). Now, they provide appointment scheduling via the My Health online patient service. The option ‘Appointment for Preventive Health Check’ has been enabled and, as of 1 August this year, is available in three Far Eastern regions — the Jewish Autonomous Region, the Republic of Buryatia, and the Republic of Sakha (Yakutia).
Over 368 thousand Far Eastern Federal District residents used the My Health service on the Public Services Portal of the Russian Federation in 2018. E-services are increasing in popularity. The number of users in the first half year of 2019 included 360 thousand residents of the Far East.

Which healthcare project implemented in the past five years in the Far East do you consider the most successful?
Far Eastern regions have become part of a high-priority project to develop air medical services. The timely transpor- tation of patients by a well-equipped ambulance helicopter manned by a well-trained healthcare team has saved about 5 thousand lives in the past two years. Since 2019, the Ministry of Health has been engaged in develop- ing air medical services as part of the Healthcare national project. 10 out of 11 Far Eastern regions are involved. In the first seven months of 2019, 762 flights were made in Far Eastern regions, evacuating 1,284 patients, including 250 children, 109 of whom were infants under the age of 1.
Perinatal care centres have been built in two Far Eastern regions — the Republic of Sakha (Yakutia) and Sakhalin Region — as part of the national programme for the development of perinatal care centres. The launch of perinatal care centres improved the quality and availability of health care for women and children in high-risk groups.
Real virtuality: Far Eastern medicine and advanced technology
Virtual reality and blockchain may become the main ways to solve the lack of access to medical services in the Far Eastern federal district.
According to the Russian Public Opinion Research Centre, 1 in 3 inhabitants in the Russian Far East is satisfied with their access to medical services, while 40% think that the region has good infrastructure and hospital equipment. Factors such as the hundreds of kilometres between populated areas, the lack of modern hospitals, and the lack of specialist personnel have forced Far Eastern authorities to use traditional methods to widen access to medicine, such as building new hospitals and high-tech medical centres, as well as unusual solutions, such as air ambulances, specialist mobile clinics (via air and railway), and advanced technology. Solutions that, not too long ago, were the stuff of sci-fi novels.
TOOL 1. Blockchain
Blockchain is technology which gives each patient (and doctors) access to their medical history and treatment at any time. The local authorities have already developed a project called ‘Creating a unified digital circuit based on the unified state information system for the healthcare sector’ that is, essentially, a virtual electronic medical history that optimizes treatment and reduces the appointment lengths. All medical institutions will be connected to this electronic chart, including paramedical stations. By 2024, all citizens of Russia will be able to use the state portal to schedule a doctor’s appointment, request a home medical visit, enquire about compulsory medical insurance and their insurance company, see what their doctor prescribed them and when (as well as the cost of procedures), and put their name down for a check-up or medical examination.
Blockchain allows the patient to collect and keep information about every diagnosis, doctor’s visit, medical procedure, prescription, test result, and sample, which can be accessed by a doctor located anywhere in the world, by the patient, and, if necessary, by a third party such as an insurance company representative. Data entered into the blockchain system cannot be amended. A doctor who is recording new information about the patient’s medical history will not be able to delete patient information that is already in the system. Blockchain prevents people from manipulating patients’ medical data with the intent of obtaining positive health assessments or fake sick notes. It also solves the problem of writing out prescriptions.

This system has already been trialled in Estonia. In Russia, it may come up against several problems, as noted in research carried out by the Higher School of Economics. For example, people don’t understand how blockchain works and don’t trust the electronic patient chart — and for good reason. If data isn’t well protected, it can be hacked into and uploaded to the web. Moreover, it’s worth considering the reluctance of medical professionals, who often grudgingly make the leap to the digital world, as well as the old computers in regional hospitals and clinics: paramedical stations in rural areas may have no computers at all. And there’s another, purely technical, problem: those uploading the data to the patient chart may be using different computer software and combining them doesn’t seem to be possible.

The Minister of Health Veronika Skvortsova (centre) and her deputy Oleg Salagai (right) at the opening of the «Healthy Life» Area with Alexander Stuglev, CEO of the Roscongress Foundation and project leader Anastasia Stolkova
TOOL 2. Virtual reality
According to a forecast by the research and consultancy firm IndustryARC, the global market for virtual technology and augmented reality in the healthcare sector will reach USD 2.54 billion by 2020.
At present, this tool is actively being used in the medical profession. First, it is used in education (e.g. broadcasting operations online, presenting clinical findings in real time, creating simulations for students and surgeons, etc.). Second, it is used for treatment purposes, such as for psychological disorders, disorders of the nervous system, and psychotherapy.
For example, doctors at the Royal London Hospital removed a cancerous growth while simultaneously streaming the entire procedure on the Web using augmented reality glasses, Google Glass, worn by the surgeon. The procedure was watched by 13,000 students (almost in real time, there was a time lag of just a few minutes). They had a unique opportunity to ask questions, which the surgeon could then see on a peripheral screen and was able to answer verbally.
Another way of using virtual reality is during the course of treatment itself, primarily to improve patients’ quality of life. One of these projects — which involves treating patients after a brain haemorrhage — was presented to the international market last year by asubsidiary of the Russian state corporation Rostec. Their neuro-simulator ReviVR was created for hospitals and clinics and uses virtual reality technology to rehabilitate patients that had suffered brain haemorrhages. Patients wear virtual reality glasses to virtually orient them in an upright position, along with an air pressure gauge to simulate the process of walking, helping repair part of the neural links damaged by the haemorrhage. This simulator costs around RUB 1.5 million.
Moreover, doctors at the Chalmers University of Technology in Sweden were able to link a patient up to an amputated arm with sensors, which captured muscle signals, transmitted them to a monitor and allowed the patient to ‘move’ the absent arm by wearing 3D glasses. The study confirmed that the patient was even able to drive a virtual vehicle.
Blockchain prostheses are being made in Russia as well. The most significant of these have been created by two start- ups: Motorika and MaxBionic. In 2017, Motorika showcased its first bionic prosthesis, called Stradivari, and there are already real patients: children with similar artificial limbs.

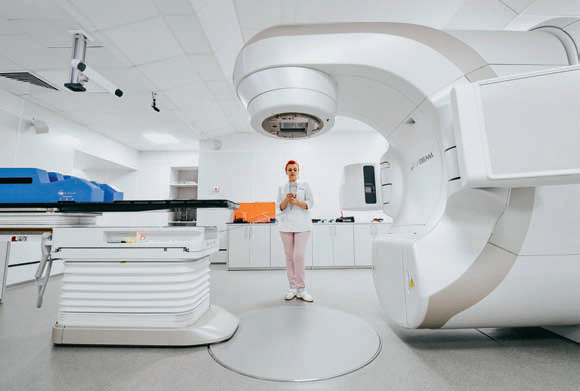
Two high-energy linear accelerators were recently installed at the Primorye Territory cancer screening centre
TOOL 3. Telemedicine
Telemedicine has been successfully undergoing development in Russia for years. On 1 January 2018, a law on telemedicine entered into force in Russia, aimed at providing patients with remote medical treatment upon diagnosis and electronic prescriptions. BBC Research valued the world telemedicine market at USD 44 billion by 2019. According to experts, the potential of the Russian market will soon exceed RUB 18 billion annually.
According to data obtained by the American Telemedicine Association, the number of ambulance patients decreased by 80% between 2008 and 2016. The number of beds occupied and in-patients fell by 19% and 25%, respectively. The reason for this is not only that appointments have moved online, but also because of the possibility of tracking a patient’s condition remotely.
Russia is already seeing the effects of introducing telemedicine. Last year, Minister of Health Veronika Skvortsova said that using telemedicine to plan routes for ambulances and critical care vehicles reduced the wait time for patients to 20 minutes in 90% of cases. Moreover, Skvortsova stressed that these results were seen not just in Moscow, but in Siberia and the Far East as well (source: https://tass.ru/obschestvo/4877691)
Russia’s own telemedicine projects include Yandex.Health and Sberbank’s DocDoc. Mobile phone providers have already launched telemedicine-based services. The fiercest competition is primarily among service aggregators, who offer a basic service allowing you to ‘video stream and chat with doctors from various clinics.’ However, contrary to hopes and expectations, telemedicine is still mainly used in Moscow and St. Petersburg, rather than in remote regions. Experts think that one of the main barriers to development in this area is patient conservatism and the reluctance of regional doctors to offer remote appointments due to concerns surrounding legal liability. This is why issues related to the integration of new technologies in the Russian Far Eastern healthcare system will be discussed at the Eastern Economic Forum (EEF 2019) on 4–6 September 2019. Furthermore, there will be an exhibition at EEF 2019 showcasing new healthcare projects.


Anastasia Stolkova,
FIRST DEPUTY DIRECTOR FOR DEVELOPMENT,
ROSCONGRESS FOUNDATION
What is Healthy Life’s goal at EEF?
Healthy Life is one of the Roscongress Foundation’s key projects. To date, activities related to the Healthy Life project have been included in the business agenda of all the Foundation’s major forums. The goal is to contribute to the development of practical solutions to improve the quality and length of the population’s healthy life expectancy.
The Far Eastern Region is unique because of the size of its constituent territories, low population density, challenging climate, the need to build mobile medical clinics and rural health posts and develop a medical air service. All this justifies the creation of a separate block in the Forum programme titled ‘New Solutions for Improving Quality of Life.’
Discussions will focus on providing medical care in remote areas and introducing new technologies in healthcare, biological safety, and public health programmes in the Far East. The Healthy Life project opens up brand new opportunities for participants in the medical and social sectors. Representatives from every community can have their voices heard and receive support in implementing their goals.
Particular attention will be paid to the development of corporate healthcare programmes in Russia. We expect our partners to announce an industry-specific competition at the upcoming Forum.
The results of all of the discussions held in the healthcare track throughout the year will be presented in February 2020 at the Healthy Life Forum. Special attention will be paid to the problems facing the Far Eastern and Arctic regions.
Do you have any surprises planned for the site? New technologies, new developments...
This is the first time that the ‘Healthy Life’ Area will be present at the Eastern Economic Forum. It aims to become a place that brings together leading representatives of the medical and scientific communities. EEF participants will be able to undergo DNA testing, visit a healthy diet bar and business networking area, and get diagnosed at the ‘Smart Express Clinic.’ The ‘Telemed-Express’ innovative mini-clinic network project is of particular social significance: new technologies make it possible for patients in the Far Eastern region region to access the best in medical care at their convenience with the use of virtual reality and telemedicine tools. This digital clinical model is a completely new type of primary healthcare that improves medical and economic efficiency in keeping with the principle of 20:80 (80% of the result for 20% of the cost). This is fully consistent with the objectives of the federal ‘Development of a Primary Healthcare System’ Project, which is part of the National Healthcare Project. An important ‘Healthy Life’ Area event will be the signing of a cooperation agreement between the National Medical Research Radiological Center of the Ministry of Health of the Russian Federation and Medical Tourism Japan Co., Ltd. It concerns the creation of the first clinical centre for the treatment of cancer patients with carbon ion radiotherapy in Russia. At present, there isn’t a single clinical centre for ion therapy in our country, although this type of treatment is developing rapidly in other parts of the world. The creation of a modern centre for ion therapy at the National Medical Research Radiological Center will guarantee the fastest possible introduction of all available options into clinical operation and their proper use.

The ‘Healthy Life’ project, launched in February 2019 with eponymous Forum held in
Sochi, has become an integral part of the Roscongress Foundation’s key events. Russian Deputy Prime Minister Tatyana Golikova inaugurated the project’s presentation area at SPIEF 2019


